COPD
COPD
Management of Chronic Obstructive Pulmonary Disease
Adapted from: O'Donnell DE, Aaron S, Bourbeau J, et al. Canadian Thoracic Society recommendations for management of chronic obstructive pulmonary disease — 2007 update. Can Respir J 2007;14(suppl B):5B–32B.
OVERVIEW
Chronic obstructive pulmonary disease (COPD) affects an estimated 4.4% of Canadians aged 35 or older, and was the fourth leading cause of death in both men and women in Canada in 2004. Persistent inflammation of the small and large airways (most often caused by smoking) leads to expiratory flow limitation, lung hyperinflation, and, ultimately, respiratory complications. A wealth of new evidence became available after the publication of the 2003 guidelines; the authors of the 2007 update reviewed the literature and provided revised and/or new recommendations for the diagnosis and treatment of this challenging condition.
KEY POINTS
KEY POINTS
- Smoking is the primary risk factor for COPD.
- Spirometry results used in combination with the Medical Research Council (MRC) dyspnea scale provide a simple means of disease stratification.
- A comprehensive COPD management strategy should include education, smoking cessation, and pharmacotherapy. Bronchodilators are the mainstay of therapy.
Definition
Definition
COPD is a respiratory disorder characterized by progressive airway obstruction, lung hyperinflation, and systemic manifestations. It is largely caused by smoking. In COPD, exacerbations gradually increase in frequency and severity over time.
Risk factors
Risk factors
Smoking is the primary risk factor for COPD, although other environmental risk factors, such as air pollution and occupational exposure, can also trigger COPD.
Assessment
Assessment
Early diagnosis and successful smoking cessation can slow progression of COPD and allow patients to begin pharmacotherapy, which can improve their symptoms and overall health status. Mass screening is not recommended, but the Canadian Lung Association recommends spirometry for all current and ex-smokers >40 years of age, who answer yes to any one of the following questions:
- Do you cough regularly?
- Do you cough up phlegm regularly?
- Do even simple chores make you short of breath?
- Do you wheeze when you exert yourself, or at night?
- Do you get frequent colds that persist longer than those of other people you know?
Disease severity
Disease severity
-
The forced expiratory volume in 1 second (FEV1) test is necessary for diagnosis of
COPD and for follow-up, but it correlates poorly with risk of mortality, as well as
with symptom intensity, exercise capacity, and quality of life. The Medical Research
Council (MRC) dyspnea scale (Table 2) better reflects overall disease among
COPD patients. The Canadian Thoracic Society recommends a simple stratification
system based on both spirometry and the MRC system (Table 3). This stratification
system still requires validation.
Differential diagnosis
Differential diagnosis
Table 4 outlines the clinical differences between asthma and COPD. The clinical features above, combined with persistent airway obstruction (demonstrated by spirometry), strongly suggest a diagnosis of COPD.
It is possible for some patients to have mixed asthma and COPD (e.g., patients with asthma plus a history of smoking). Patients with mixed disease will need individualized education and self-management plans, and will likely need different goals and treatment expectations than those with either disease alone.
MANAGEMENT
MANAGEMENT
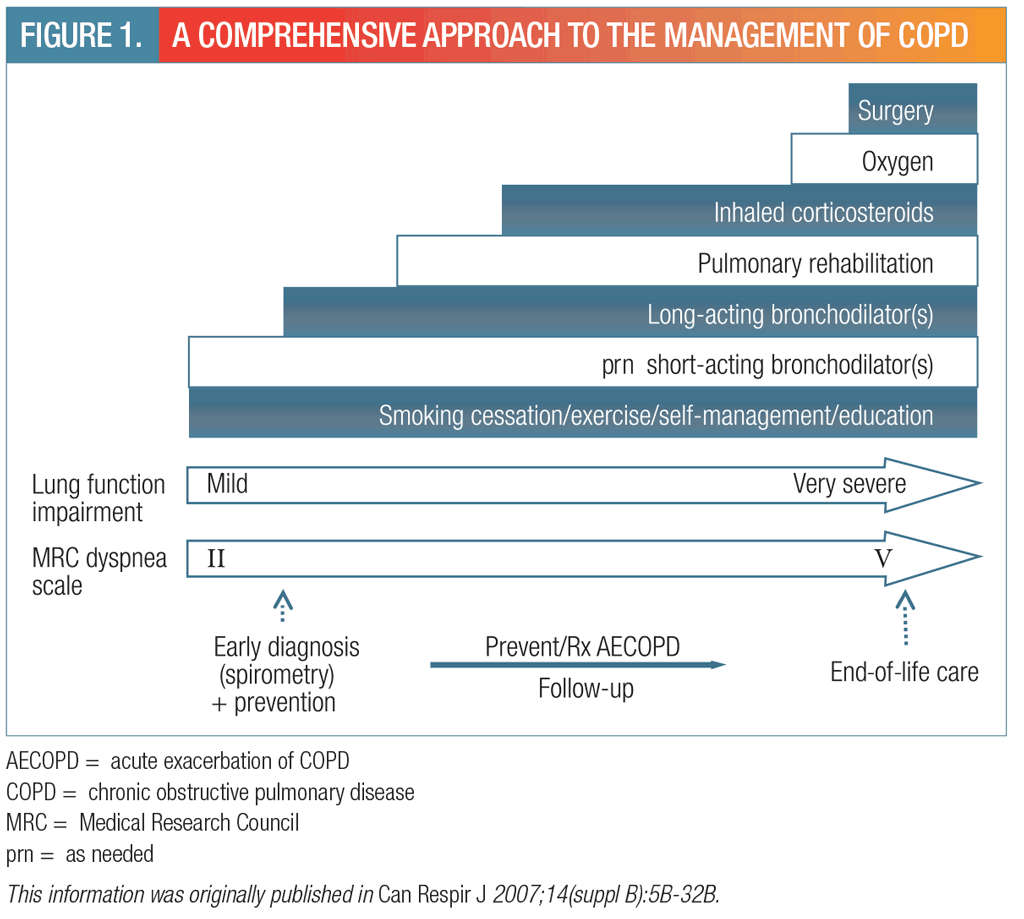
The goals of COPD management are to prevent disease progression, reduce the frequency and severity of exacerbations, alleviate symptoms, improve exercise tolerance, treat exacerbation and complications, improve overall health, and reduce mortality. A comprehensive management strategy should include an educational component, smoking cessation, and pharmacotherapy (Figure 1).
Education
Education
Education should be individualized depending on disease severity, and should include both the patient and his/her family. Interventions should include diseasespecific information, self-management principles, smoking cessation, and strategies to alleviate dyspnea.
Smoking cessation
Smoking cessation
Patients should be advised to quit smoking and be offered pharmacotherapy for smoking cessation whenever possible.
Pharmacotherapy
Pharmacotherapy
Bronchodilators are the mainstay of therapy for COPD. Recommendations for pharmacotherapy are as follows (Figure 2):
- Mild: short-acting bronchodilator as needed; some patients may derive benefit from a long-acting bronchodilator.
- Moderate-to-severe persistent symptoms: long-acting bronchodilator (e.g., tiotropium) plus short-acting beta2-agonist as needed.
- Moderate-to-severe persistent symptoms, infrequent exacerbations: tiotropium and a long-acting beta2-agonist (LABA), plus short-acting beta2- agonist as needed.
- Moderate-to-severe persistent symptoms, history of exacerbations: tiotropium, LABA and inhaled corticosteroid (ICS), plus short-acting beta2- agonist as needed; ICS should be used only in combination with a LABA.
- Severe symptoms, despite tiotropium and a LABA/ICS: long-acting theophylline (with careful monitoring of blood levels, side effects and potential drug interactions).
Long-term treatment with oral corticosteroids is not recommended.
Acute exacerbations
Acute exacerbations
Prevention of acute exacerbations
- Strategies for the prevention of acute exacerbations of COPD include the following:
- Smoking cessation.
- Annual influenza vaccination for those in whom it is not contraindicated.
- Pneumococcal vaccination (at least once; in high-risk patients, consider repeating in 5 to 10 years).
- Consider treatment with tiotropium ± a LABA in patients with FEV1 <60%.
- Consider treatment with LABA + ICS in patients with FEV1 <60% and who experience one or more acute exacerbations per year.
Management of acute exacerbations
- Management approaches for acute exacerbations should include the following:
- Diagnostic evaluation, including a complete history and physical examination
to rule out other possible causes of dyspnea.
- Arterial blood gases in patients with low arterial oxygen saturations.
- Chest radiography for patients who present to the emergency department or for hospital admission.
- Gram stain and culture for patients with purulent sputum and very poor lung function, frequent exacerbations, or antibiotics in the preceding three months.
- Pulmonary function tests in patients who have not previously had spirometry.
- Inhaled bronchodilators to relieve dsypnea.
- Oral or parenteral corticosteroids.
- Antibiotics in patients with purulent exacerbations.
Other management options
Other management options
Pulmonary rehabilitation
- All patients should be encouraged to maintain an active lifestyle and be cautioned about the consequences of inactivity for their disease.
- Patients with dyspnea and limited exercise capacity, despite pharmacotherapy,
should be referred for supervised pulmonary rehabilitation. Criteria
for referral:
- Clinically stable
- Reduced activity levels and increased dyspnea despite pharmacotherapy
- No evidence of active ischemic, musculoskeletal, psychiatric, or other systemic disease
- Sufficient motivation for participation
- More pulmonary rehabilitation programs are urgently needed across Canada; the existing programs are able to serve only about 1.2% of the current population of patients with COPD.
Oxygen therapy
Patients with stable COPD and severe hypoxemia (PaO2 ≥55 mm Hg) — or PaO2 <60 mm Hg plus bilateral ankle edema, cor pulmonale or hematocrit >56% – should be offered long-term continuous oxygen.
Noninvasive positive pressure ventilation
Patients with milder exacerbations do not generally benefit from noninvasive positive pressure ventilation (NPPV), but NPPV should be considered in patients with a severe exacerbation (pH <7.3). NPPV is not indicated for patients to whom the following characteristics apply:
- Respiratory arrest
- Hemodynamic instability
- High risk for aspiration
- Impaired mental status
- Other inability to cooperate
Surgery
Criteria for lung transplant include the following:
- FEV1 <25% predicted (without reversibility)
- Partial pressure of arterial CO2 >55 mm Hg
- Elevated pulmonary artery pressures with progressive deterioration
Alpha-antitrypsin deficiency
- Alpha antitrypsin (AAT) replacement therapy should be restricted to patients with an FEV1 >35% and <65% predicted, who have quit smoking and are on optimal pharmacotherapy but continue to show a rapid decline in FEV1.
CONCLUSION
CONCLUSION
COPD is a largely preventable and treatable disease. New research has increased understanding of COPD, giving physicians the ability to diagnose it earlier and offer more effective management/treatment strategies to those who suffer from this complex condition.
Addendum
Addendum
Since the publication of the guidelines in 2007, roflumilast, a phosphodiesterase-4 (PDE4) inhibitor, has been approved by Health Canada as an add-on therapy to bronchodilator treatment for the maintenance treatment of severe disease.* Use of PDE4 inhibitors is discussed in the 2012 Global Strategy for the Diagnosis, Management and Prevention of Chronic Obstructive Lung Disease (GOLD) guidelines.†
*Daxas [product monograph]. Oakville, ON: Takeda (Nycomed) Canada; 2010.
†Vestbo J, Hurd SS, Agusti AG, et al. Global Strategy for the Diagnosis, Management and Prevention of Chronic Obstructive Pulmonary Disease, GOLD Executive Summary. Am J Respir Crit Care Med 2012 Aug 9 [epub ahead
of print].
Full guidelines
Full guidelines
The preceding material represents a summary of the 2007 update to the Canadian Thoracic Society recommendations for management of chronic obstructive pulmonary disease. Clinicians are encouraged to consult the complete document (see O'Donnell DE, Aaron S, Bourbeau J, et al. Canadian Thoracic Society recommendations for management of chronic obstructive pulmonary disease – 2007 update. Can Respir J 2007;14(suppl B):5B–32B).