GOUT

GOUT
Management of Gout and Hyperuricemia
Adapted from: Khanna D et al. American College of Rheumatology guidelines for management of gout. Part 1: Systematic nonpharmacologic and pharmacologic therapeutic approaches to hyperuricemia. Arthritis Care Res 2012;64(10):1431-46.
OVERVIEW
Gout is a common inflammatory arthritic disease resulting from elevated serum monosodium urate. It affects approximately 3% of Canadian adults.1 Gout prevalence has been on the rise, due in part to the aging of the North American population and the increased prevalence of a number of conditions that lead to hyperuricemia. Health-related quality of life is reduced among gout sufferers, especially as symptom severity and attack frequency increase.2 Gout continues to present a challenge to many health care practitioners despite the availability of effective therapies.
The new expert consensus guidelines from the American College of Rheumatology were published in two parts. The first paper, on which this summary is based, makes recommendations for management of hyperuricemia and chronic gouty arthritis. The second paper discusses the control of pain and inflammation in acute attacks, as well as prophylaxis.3
KEY POINTS
KEY POINTS
- Gout carries a risk of long-term morbidity and impaired quality of life.
- Risk factors for gout include hyperuricemia, male sex, and several established cardiovascular risk factors.
- The diagnosis is typically made clinically. Hyperuricemia is not diagnostic as serum urate may be normal during attacks and some individuals with elevated levels do not develop gout.
- Clinicians should evaluate symptom severity and burden as well as risk factors and comorbidities in each patient.
- The treatment goals during an acute attack are to reduce pain, swelling and disability.
- The recommended serum urate target is <6mg/dL; a target of <5mg/dL may be necessary to improve disease signs and symptoms in some patients.
- A xanthine oxidase inhibitor (allopurinol or febuxostat) is the recommended first-line therapy for reducing serum uric acid.
- Lifestyle measures and management of comorbid conditions are also recommended to reduce hyperuricemia and the likelihood of gout attacks.
Diagnosis and evaluation
Diagnosis and evaluation
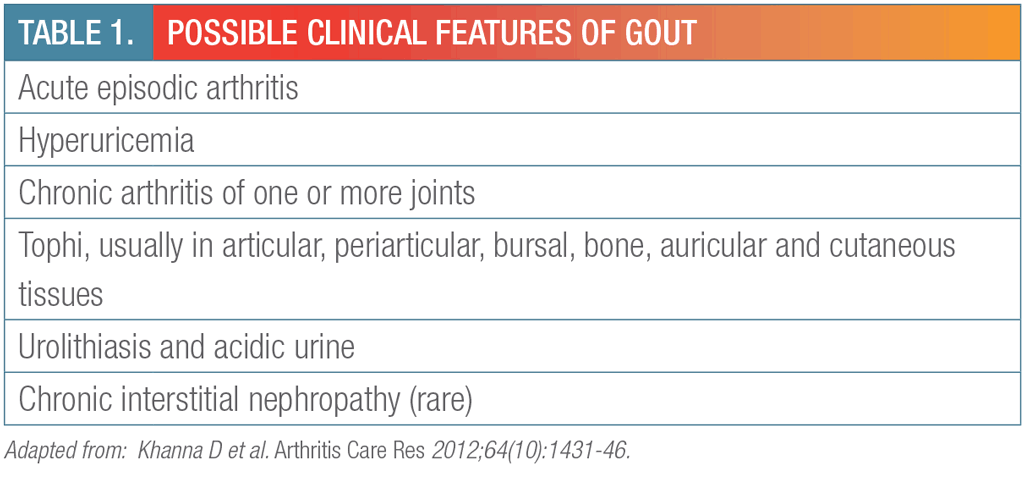
Gout usually presents with an acute, self-limited episode of painful swelling and redness affecting a single joint (often, the first metatarsophalangeal joint). It can progress to chronic arthritis of multiple joints (Table 1). Tophi — tissue deposits of monosodium urate crystals — may be observed on physical examination, imaging or pathologic examination.
The diagnosis may be made clinically, based on typical signs and symptoms of pain, swelling and erythema. Detection of urate crystals in synovial fluid or aspirated from a tophus permits a definitive diagnosis but is not always needed/available in clinical practice. Culture of synovial fluid may assist detection of co-existing septic arthritis. X-rays are not typically useful for diagnosis of acute attacks.4
Clinicians should perform an evaluation of symptom severity and burden as well as risk factors and comorbidities, with a complete history and physical examination.
Risk factors
Risk factors
Clinical research studies have identified numerous risk factors for gout (Table 2). Men are about 7 times more likely than women to develop gout. The prevalence of the disease rises with age; up to 7% of men aged >65 and 3% of women >85 are affected.4
As part of overall management of gout, clinicians should consider the reasons for hyperuricemia in each patient and possible additional measures to alleviate it, such as intensified or altered treatment of risk factors and comorbid conditions.
Treatment
Treatment
For acute attacks, the goal is relief of pain and associated symptoms. Oral colchicine or a nonsteroidal anti-inflammatory drug (NSAID) is typically used as first-line therapy.3
Figure 1 summarizes the ACR management plan for patients with a confirmed diagnosis of gout, which includes lifestyle measures and medications for lowering hyperuricemia. Patient education about diet and lifestyle choices can help prevent gout attacks and promote overall health and management of comorbid conditions (Table 3).
The aim should be to lower serum urate to <6 mg/dL; achievement of a level <5 mg/dL may be necessary to improve disease signs and symptoms in some patients, such as those with tophi observed on clinical evaluation or diagnosed with chronic tophaceous gouty arthopathy.
Allopurinol and febuxostat, titrated to maximum appropriate dose, are the recommended first-line medications. Probenecid is an alternative for patients in whom a xanthine oxidase inhibitor is contraindicated or not tolerated; however, it is not appropriate for patients with creatinine clearance <50 mL/min.
Serum urate lowering therapy can begin during an acute attack provided that an anti-inflammatory agent has been initiated. If the patient's serum urate does not reach the target with the maximum appropriate dose of a first-line agent and there is continued disease activity, the other may be substituted; subsequently, a uricosuric agent (probenecid) and then pegloticase may be considered as additional therapy.
Serum urate should be monitored every 2-5 weeks during titration of urate lowering therapy, and approximately twice yearly once the target level is achieved.
CONCLUSION
CONCLUSION
The new ACR guidelines are designed to address identified gaps in the managemof gout and to reflect the introduction of new therapeutic options. Patient education ion about the importance of adherence to lifestyle and pharmacologic therapies remains a mainstay of management.
References and Supplementary Resources
References and Supplementary Resources
-
Badley E, Desmeules M. Arthritis in Canada – An Ongoing Challenge. Public Health Agency of Canada. www.phac-aspc.gc.ca/publicat/ac/ac_2e-eng.php, accessed September 30, 2012.
-
Khanna P et al. Tophi and frequent gout flares are associated with impairments to quality of life, productivity, and increased healthcare resource use: Results from a cross-sectional survey. Health Qual Life Outcomes 2012;10(1):117.
-
Khanna D et al. American College of Rheumatology guidelines for management of gout. Part 2: therapy and anti-inflammatory prophylaxis of acute gouty arthritis. Arthritis Care Res 2012;64(10):1447-61.
-
Zhang W et al. EULAR evidence-based recommendations for gout. Part I: Diagnosis. Report of a task force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis 2006;65:1301-11.
Full guidelines
Full guidelines
The preceding material is a summary of part 1 of the 2012 ACR guidelines on gout, specifically on the management of hyperuricemia. For details, clinicians are advised to consult the full guidelines:
Khanna D et al. American College of Rheumatology guidelines for management of gout. Part 1: Systematic nonpharmacologic and pharmacologic therapeutic approaches to hyperuricemia. Arthritis Care Res 2012;64(10):1431-46.
Khanna D et al. American College of Rheumatology guidelines for management of gout. Part 2: therapy and anti-inflammatory prophylaxis of acute gouty arthritis. Arthritis Care Res 2012;64(10):1447-61.