HYPERTENSION
HYPERTENSION
Diagnosis and Management of Hypertension
Adapted from: Adapted from Daskalopoulou SS et al. The 2012 Canadian Hypertension Education Program (CHEP) recommendations for the management of hypertension: blood pressure measurement, diagnosis, assessment of risk, and therapy. Can J Cardiol 2012;28(5):270-87; Canadian Hypertension Education Program slide kits: 2012 Canadian recommendations for the management of hypertension. What's new? What's still really important? Recommendations for hypertension treatment.
OVERVIEW
Hypertension is a significant and common risk factor for cerebrovascular, coronary artery disease (CAD) and peripheral vascular disease, heart failure, renal failure, dementia, and atrial fibrillation. Each year, the Canadian Hypertension Education Program (CHEP) provides updated evidence-based recommendations aimed at optimizing blood pressure (BP) management.
With each update, CHEP focuses on specific areas in which improvements in clinical care are needed. In 2012, the focus was on prevention of hypertension through timely assessment, modifying patients' exposure to risk factors, and lifestyle intervention.
KEY POINTS
KEY POINTS

Screening and diagnosis
Screening and diagnosis
The BP of adult patients should be measured with standardized techniques at all appropriate clinic visits, so that hypertension can be identified early and cardiovascular risk assessed. If BP is high at an initial clinic visit, additional measurements (as shown in Figure 1) are required to confirm the diagnosis of hypertension. Patients with "high normal" BP (130-139/85-89 mm Hg) should be assessed annually. Home BP monitoring, as per the suggested protocol in Table 1, can be considered in the place of 24-hour ambulatory monitoring, for example to identify patients with possible "white-coat" BP elevations.
Global vascular risk
Global vascular risk
Most Canadians with hypertension also have other cardiovascular risk factors. One in 2 younger hypertensive Canadians (i.e., aged < 45 years) with multiple cardiovascular risks are currently not treated with anthypertensive agents.
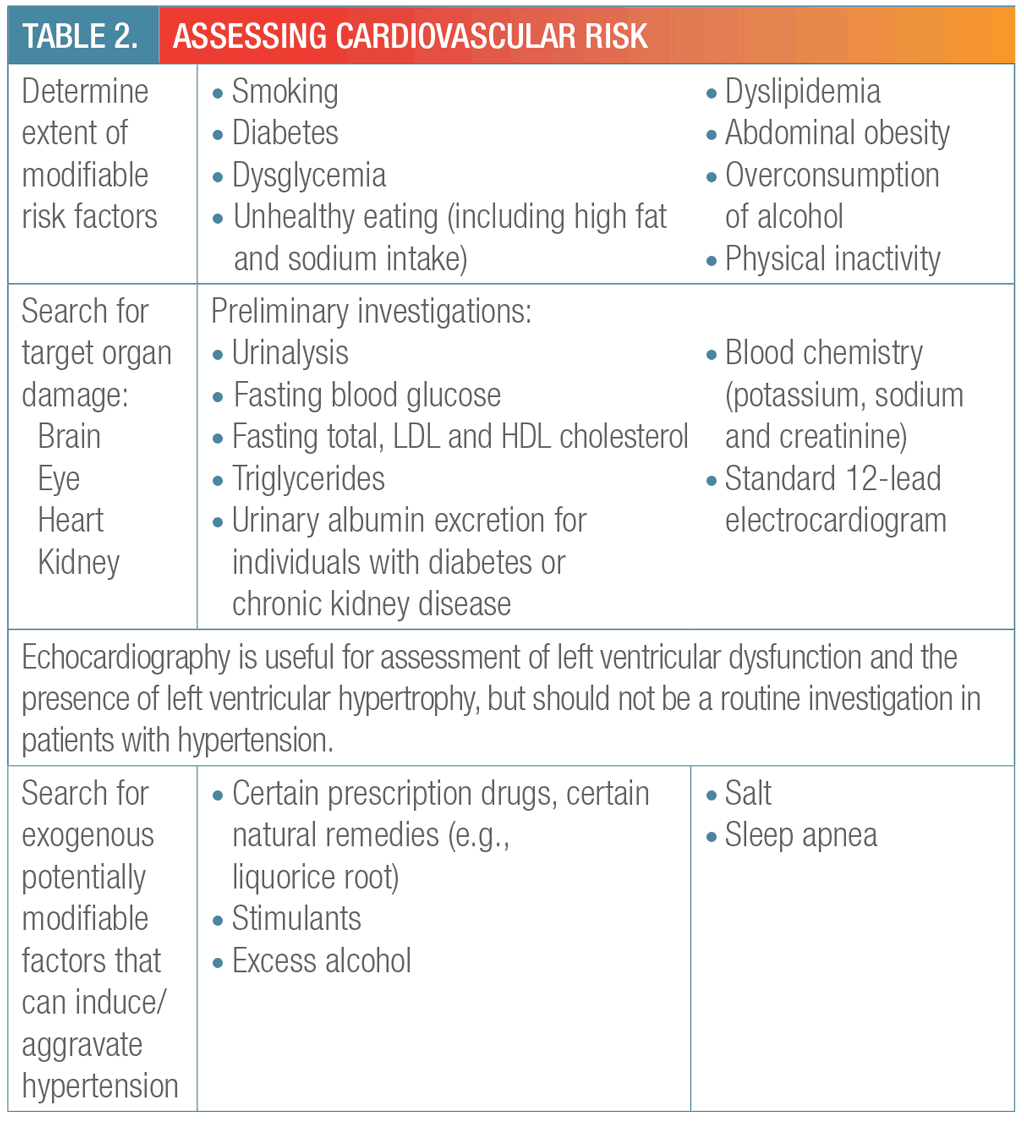
Global cardiovascular risk should be assessed (Table 2). Tools such as the Framingham Heart Study model (http://www.framinghamheartstudy.org/risk/ hrdcoronary.html) or Systematic Cerebrovascular and Coronary Risk Evaluation Canada (www.scorecanada.ca) may be employed.
Clinicians should ensure vascular protection in all people with hypertension.
Patients with heightened cardiovascular risk (3 or more risk factors) or with atherosclerotic disease should also receive statin therapy. Low-dose ASA is also advisable for patients at elevated cardiovascular risk whose BP is controlled.
Management
Management
Role of lifestyle modification
A program of lifestyle modification is the primary step in the prevention and management of hypertension and cardiovascular disease. CHEP recommends numerous measures to reduce the likelihood of hypertension, reduce BP, and decrease the risk of cardiovascular complications in people who have elevated BP (see below). In patients with diabetes and BP >130/80 mm Hg, lifestyle interventions should be initiated concurrently with pharmacologic therapy. In low-risk patients with stage 1 hypertension (140-159/90-99 mm Hg), lifestyle modification can be the sole therapy.
- A healthy diet: high in fresh fruits and vegetables, low-fat dairy products, dietary and soluble fibre, whole grains and protein from plant sources; low in saturated fat, cholesterol, and salt in accordance with Canada's Guide to Healthy Eating or the DASH diet
- Regular physical activity: accumulation of 30-60 minutes of moderateintensity dynamic exercise (walking, jogging, cycling, swimming) 4-7 days per week, in addition to daily activities
- Low-risk alcohol consumption (<2 standard drinks/day and less than 14/week for men and less than 9/week for women
- Attaining and maintaining ideal body weight (BMI 18.5-24.9 kg/m2)
- A healthy waist circumference: < 102 cm for men, < 88 cm for women
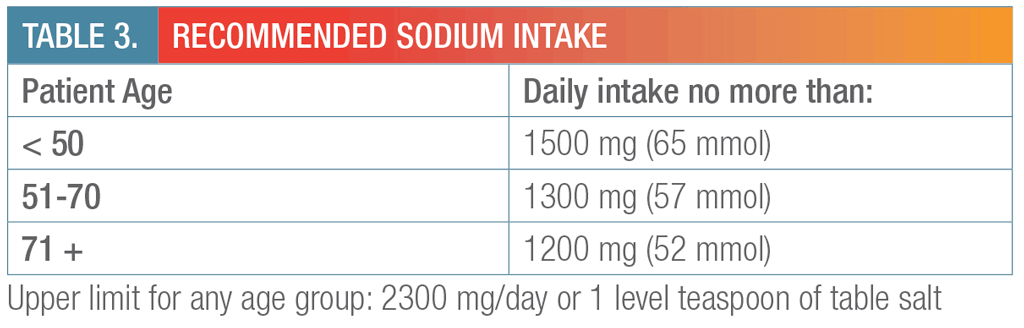
- Reduction in sodium intake to levels recommended by Healthy Canada (Tables 3 and 4)
- A smoke-free environment
- Stress management
It can be difficult for patients to initiate and maintain healthy lifestyle changes. Follow-up conversations about the positive impact of lifestyle measures can help keep the patient motivated.
Treat to target
Treat to target
Cardiovascular disease reduction is most successful if BP is lowered to the targets in Table 5.
The algorithms in Figures 2 and 3 illustrate the usual approach for hypertensive patients without compelling indications for a particular pharmacotherapy. Combination therapies (involving both lifestyle and drugs) are generally necessary to achieve target BP. Most people require 2 or more antihypertensive agents; this combination should be initiated immediately in patients with BP >20/10 mm Hg above target. Lower doses of multiple drugs may be more effective and better tolerated than higher doses of fewer drugs.
Figure 2.
FIGURE 2. TREATMENT OF ADULTS WITH SYSTOLIC/DIASTOLIC HYPERTENSION WITHOUT OTHER COMPELLING INDICATIONS
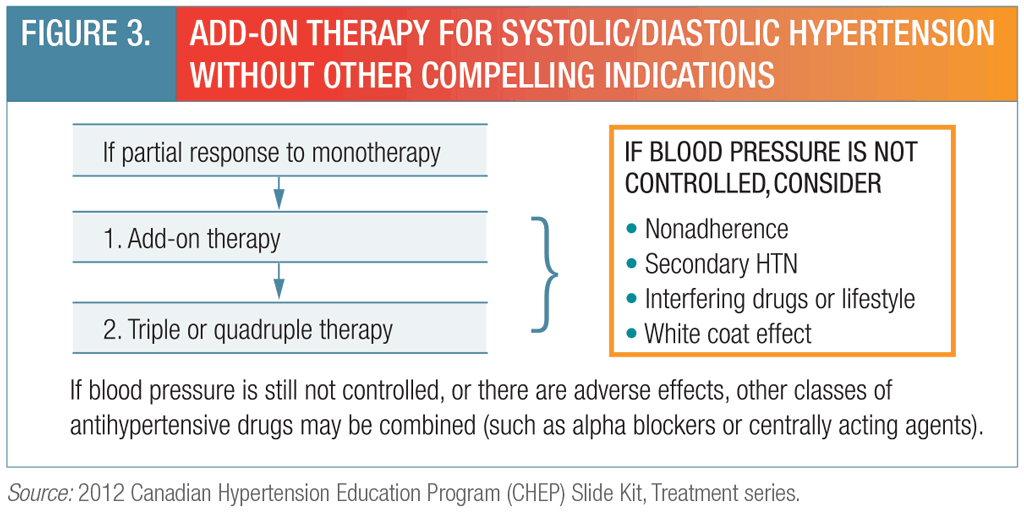
Figure 3.
FIGURE 3. ADD-ON THERAPY FOR SYSTOLIC/DIASTOLIC HYPERTENSION WITHOUT OTHER COMPELLING INDICATIONS
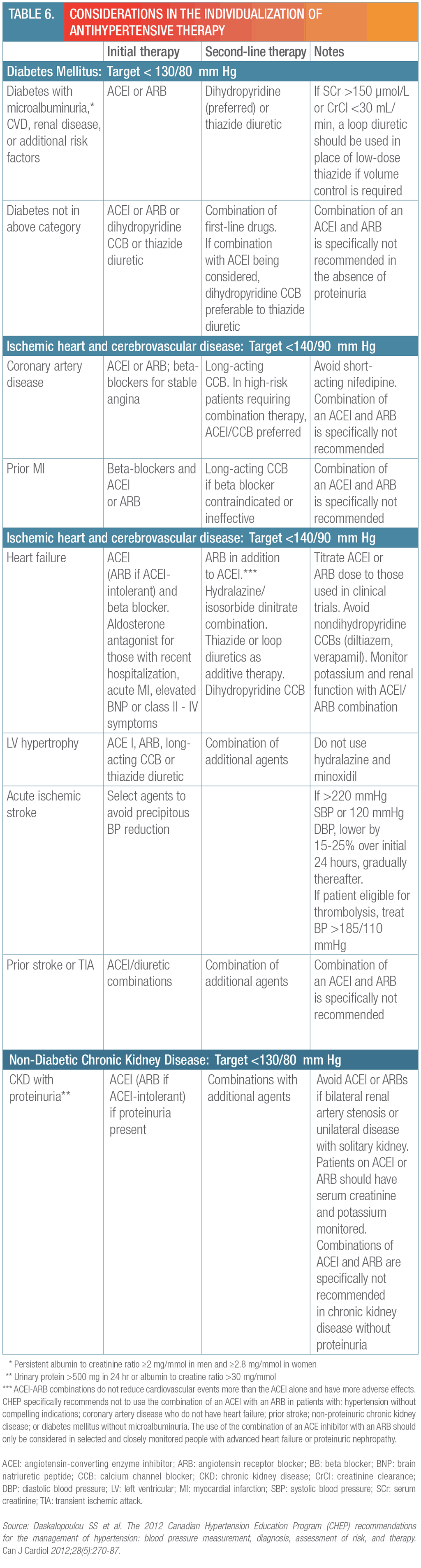
CHEP also makes specific recommendations for first-line therapies in patients with concomitant diseases (Table 5). Based on data from the ONTARGET trial, a new recommendation is that most patients with ischemic heart disease should receive an angiotensin-converting enzyme inhibitor (ACEI) or angiotensin receptor blocker (ARB) (in patients with heart failure, ACEI are preferred). In addition, based on the ACCOMPLISH trial results, CHEP indicates that for selected high-risk individuals with CAD, the combination of an ACEI and calcium channel blocker (CCB) should be considered.
Focus on adherence
Focus on adherence
Several strategies can improve patient adherence:
- Tailoring medication schedules to patients' individual daily habits
- To limit pill burden, the use of once-daily dosing and single-pill or fixeddose combination medications
- Utilizing unit-of-use packaging (several medications packaged so as to be taken together)
- Using a team approach (e.g., collaborating with a pharmacist)
Home monitoring
Home monitoring
The patient should be encouraged and assisted to become more knowledgeable about his/her global cardiovascular risk and involved in his or her own treatment. The use of a home BP monitor promotes greater patient autonomy, involvement, and responsibility for BP control. Periodic reassessment of technique and retraining is desirable. Some patients may be interested in additional electronic resources such as BP tracking "apps."
Clinicians can improve their own BP management strategies by implementing the following:
- Regularly assessing patients' compliance with lifestyle and pharmacological therapy: patients with BP above target should be seen at least every 2 months
- Maintaining contact with the patient by phone or mail, especially over the first 3 months of therapy
- Using a multidisciplinary team approach, such as asking the patient's local pharmacist or a nurse at his place of employment to help monitor adherence
- Utilizing electronic medication compliance aids
CONCLUSION
CONCLUSION
Current data indicate hypertension management has improved in Canada over the past decade, coincident with the dissemination by CHEP of up-to-date information on the benefits of and best practices for blood pressure control. Given an expected increase in the prevalence of cardiovascular disease, the importance of attention and adherence to these evidence-based guidelines and control of other risk factors cannot be overemphasized.
Hypertension and C-CHANGE
Hypertension and C-CHANGE

Patients with cardiovascular disease risk factors, such as diabetes, hypertension, and dyslipidemia, are at significantly increased lifetime risk for macrovascular events such as stroke and myocardial infarction. Consequently, patients should have all of their risk factors treated to their risk appropriate treatment targets.
The C-CHANGE (Canadian Cardiovascular HArmonization of National Guidelines Endeavour) Collaboration suggests that all cardiovascular disease risk factors should be addressed. Ideally, all patients should be stratified with respect to the cardiovascular event risk and should be at or below all their cardiovascular disease risk factors treatment targets.
Without doubt, it may be easier to treat one cardiovascular disease risk factor to target in one patient versus another and not all patients will achieve their treatment targets for all their risk factors. However, a concerted effort should be made to get most patients to or below most of their risk factors targets through a combination of heart-healthy behaviours and pharmacological therapies. Addressing all the cardiovascular disease risk factors present in any single patient and ensuring each is treated, preferably to or below target, is likely to have a greater impact on patient outcomes than treating any single risk factor perfectly while the others remain untreated or significantly undertreated.
Please refer to the C-CHANGE section in this publication for additional information.
Full guidelines
Full guidelines
The preceding material is a summary of the 2012 CHEP guidelines. Clinicians are encouraged to consult the full guidelines and accompanying educational material available at www.hypertension.ca.